Cost-Benefit of Digital Sensors in Dental Chairs
The True Cost and Benefit of Integrated Digital Sensors
For any modern dental practice, the decision to upgrade equipment hinges on a single question: will the investment pay for itself? This is especially true for core diagnostic tools like X-ray systems. While traditional film X-rays have been a staple for decades, integrated digital intraoral sensors represent a significant leap forward. But are they worth the upfront cost? The answer is a definitive yes, provided the implementation is planned strategically. A thorough cost-benefit analysis reveals that digital sensors deliver a powerful return on investment (ROI) by enhancing diagnostic speed, improving clinical accuracy, and streamlining daily operatory workflow.
This article provides a data-driven breakdown for clinic decision-makers, moving beyond the spec sheets to focus on tangible financial and clinical outcomes. We will analyze the direct cost savings, the impact on efficiency and revenue, and the critical steps for successful integration.
From Film and Chemicals to Pixels and Efficiency
Traditional radiography, with its reliance on physical film, chemical developers, and darkrooms, introduces significant operational friction into a dental practice. The process is fraught with recurring costs and workflow delays that can hinder a clinic’s productivity and profitability.
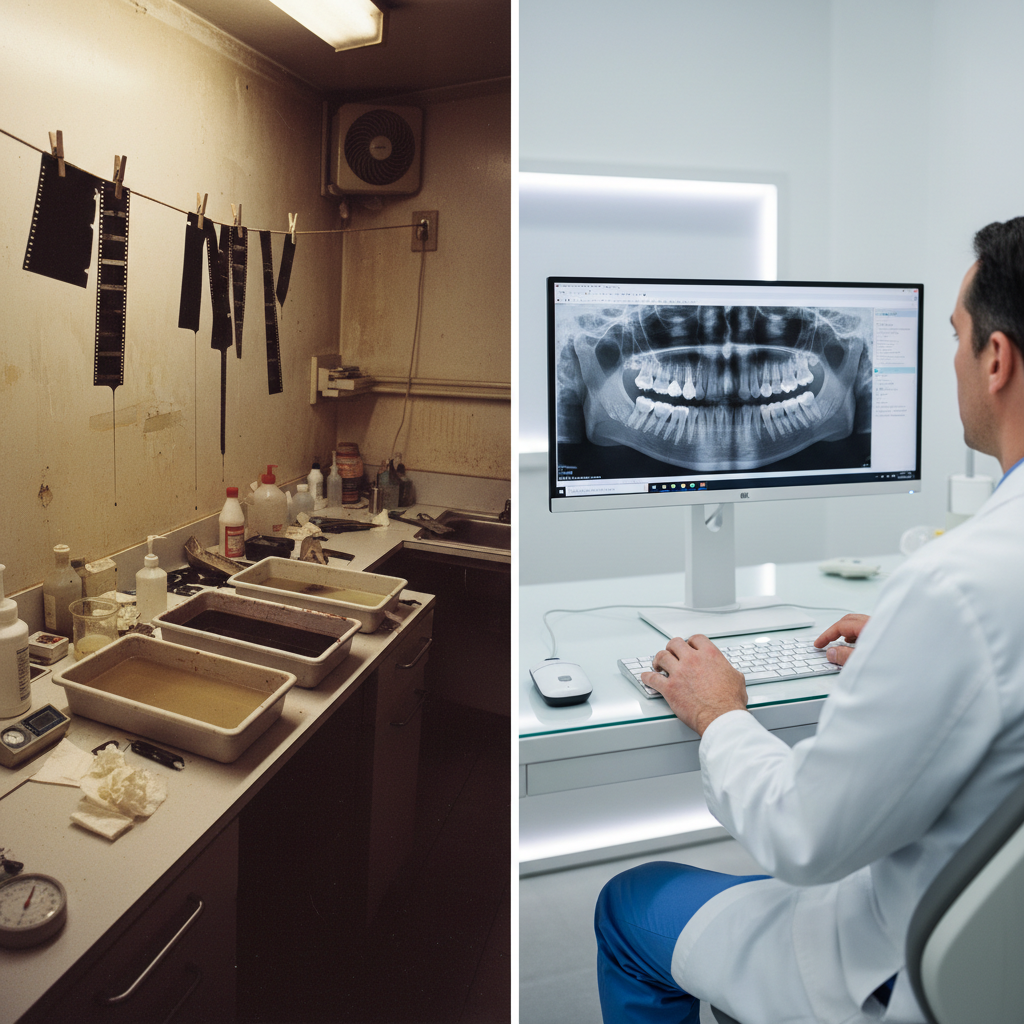
The Limitations of Traditional Film Radiography
The drawbacks of film extend beyond just the consumable costs. The entire workflow is time-consuming, requiring several minutes to process a single image. This waiting period occupies the time of both the patient and the clinical staff, extending appointment durations and limiting the number of patients that can be seen in a day. Furthermore, the quality of film X-rays is static; it cannot be adjusted or enhanced, and the images are susceptible to degradation over time. Physical storage demands space and creates administrative burdens, while sharing images with specialists or insurance providers is a cumbersome, manual process.
The Digital Advantage: Speed, Clarity, and Control
Digital intraoral sensors eliminate these challenges entirely. By capturing images and rendering them on a screen in seconds, they provide immediate diagnostic information. This speed is a cornerstone of the technology’s value proposition. The ability to instantly retake a poorly positioned shot without repeating a lengthy development process is a significant efficiency gain. According to data from practicing clinicians, a well-implemented digital sensor workflow can reduce radiographic retakes by 30-60% after an initial training period.
Moreover, digital images offer superior diagnostic capabilities. Software allows for magnification, contrast adjustment, and annotation, helping clinicians identify pathologies that might be missed on film. This level of detail supports more accurate diagnoses and more effective treatment planning, directly contributing to better patient outcomes. The digital format also simplifies compliance with regulations for quality management systems, such as those outlined in ISO 13485:2016, which mandates controlled processes for medical device handling and documentation.
Quantifying the Return on Investment (ROI)
While the initial purchase price of a digital sensor system is higher than that of a traditional setup, the long-term financial benefits are substantial. The ROI is driven by eliminating consumable costs, increasing procedural efficiency, and improving diagnostic value.
Cost Comparison: Digital Sensors vs. Traditional Film
A direct comparison reveals a clear financial advantage for digital sensors over a 5-year period. The bulk of the cost for digital is in the initial investment, while film requires continuous spending on consumables.
| Cost Factor | Digital Sensor System | Traditional Film System | Analysis |
|---|---|---|---|
| Initial Investment | High (Sensor, Software) | Low (Processor, Mounts) | Digital requires a significant upfront capital expense. |
| Consumable Costs | Very Low (Barrier Sleeves) | High (Film, Chemicals, Mounts) | This is where digital provides major long-term savings. |
| Maintenance Costs | Low (Calibration, Sleeves) | Moderate (Chemical Disposal, Processor Service) | Digital systems have fewer moving parts and require less maintenance. |
| Staff Time / Labor | Low (Immediate Image Capture) | High (Film Processing, Filing, Duplicating) | Time savings translate directly into higher clinic productivity. |
| Total Cost over 5 Years | Lower | Higher | When accounting for all factors, digital is the more cost-effective choice. |
Calculating Your Clinic’s ROI
Based on extensive clinical experience, a practice that performs more than 15 intraoral X-rays per week can often recover the full cost of a digital sensor system within 12 to 24 months. This calculation is based on time savings per exposure, the elimination of film and chemical costs, and the revenue gained from increased patient throughput.
For a detailed look at how to structure your technology budget, consider exploring Cost-Effective Dental Chair Integration Strategies, which can help you plan for a seamless transition.
Critical Success Factors for Sensor Integration
Simply purchasing a digital sensor is not a guarantee of success. The most significant returns are realized when the technology is integrated thoughtfully into the clinic’s existing infrastructure and workflows. I have seen many practices make avoidable mistakes that limit their ROI and lead to frustration.
Myth Debunked: “The Sensor is Plug-and-Play”
A common misconception is that a USB sensor can be plugged in and used effectively immediately. In reality, success depends on meticulous planning before the purchase. A failure to account for ergonomics and workflow is the most common pitfall I’ve observed. This includes verifying chair mounting options to ensure the sensor holder can be positioned correctly without straining the operator or patient. Cable routing is another critical detail; improperly managed cables are a leading cause of premature sensor failure.
Pre-Purchase Integration Checklist
To avoid these issues, every clinic should complete a pre-purchase audit. This ensures that the new technology will enhance, not hinder, your practice.
- Software Compatibility: Verify that the sensor’s drivers and software are fully compatible with your current Practice Management Software (PMS). Confirm it supports the DICOM standard for universal image formatting.
- Ergonomics and Mounting: Assess your dental chairs. Are there existing mounts for a sensor holder? Will the placement allow for efficient and ergonomic use? Planning this can improve operator comfort and Boost Clinic Productivity.
- Wired vs. Wireless: For high-volume clinics, wired sensors are generally more reliable and eliminate the workflow interruptions associated with battery management. Wireless sensors may offer flexibility but can be less suitable for back-to-back procedures.
- Staff Training Plan: Technology is only as good as the team using it. Budget for comprehensive, hands-on staff training. A dedicated 4-6 week period for training and protocol refinement is realistic to achieve consistent, high-quality images.
- Contingency Planning: Sensors are durable but not indestructible. Formulate a plan for potential downtime. This may involve a spare sensor or a service-level agreement (SLA) with your supplier for rapid replacement.
Training, Calibration, and Lifecycle Management
Achieving excellent diagnostic results requires precision. The goal of training should be to achieve positioning variability under 5 mm and angulation variance within ±5°. This level of consistency is what maximizes diagnostic value and minimizes retakes.
Long-term ownership costs are minimal but essential. This includes a budget for single-use barrier sleeves for infection control, periodic sensor calibration as recommended by the manufacturer, and eventual replacement. A busy practice should plan for a sensor lifecycle of 5 to 7 years. It’s crucial to follow manufacturer guidelines for disinfection—never autoclave a sensor, as this will destroy it. Adherence to these quality and maintenance procedures aligns with the principles found in FDA regulations like 21 CFR Part 820, which governs medical device quality systems.
Thinking about the long-term view is essential for Future-Proofing Your Operatory for New Technology.
Key Takeaways
Investing in integrated digital X-ray sensors is one of the most impactful financial and clinical decisions a modern dental practice can make. The transition from film to digital offers a clear and compelling ROI, but this return is not automatic. It is unlocked through strategic planning and thoughtful implementation.
- Financial Advantage: Digital sensors significantly lower long-term operational costs by eliminating film and chemical expenses. For most practices, the ROI is achieved within 12-24 months.
- Clinical Efficiency: The immediate image capture and reduced retake rates streamline workflow, shorten appointment times, and increase the clinic’s overall capacity.
- Diagnostic Excellence: Superior image quality and digital enhancement tools lead to more accurate diagnoses, better treatment outcomes, and improved patient communication.
- Integration is Key: Success hinges on pre-purchase planning, including software compatibility checks, ergonomic assessments, and robust staff training. Do not underestimate the importance of these foundational steps.
By viewing the adoption of digital sensors as a strategic integration project rather than a simple equipment purchase, dental clinics can maximize their return and solidify their position as modern, efficient, and patient-focused providers.
Disclaimer: This article is for informational purposes only and does not constitute professional medical or financial advice. Clinic owners should consult with financial advisors and equipment specialists to assess their specific needs and circumstances. Always follow manufacturer guidelines and regulatory standards when operating medical equipment.






