A Deep Dive into Dental Chair Waterline Management
The Hidden Risk in Plain Sight: A Deep Dive into Dental Chair Waterline Management
Every dental practice is built on a foundation of trust, where patients assume a sterile and safe environment. While instruments are meticulously sterilized and surfaces are disinfected, a significant, often overlooked, risk resides within the dental chair itself: the dental unit waterlines (DUWLs). These narrow tubes can become breeding grounds for bacteria and biofilm, posing a potential health risk.
This guide provides a comprehensive, evidence-based framework for managing DUWLs effectively. We will explore the science behind biofilm, detail practical daily and weekly protocols, evaluate modern treatment technologies, and establish a clear path for monitoring and verification, ensuring your practice not only meets but exceeds patient safety standards.
Understanding the Threat: Biofilm in Dental Unit Waterlines
The water that cools high-speed handpieces and irrigates surgical sites must be free of harmful microorganisms. However, the very design of dental chairs—with their long, narrow-bore plastic tubing and periods of stagnation—creates an ideal environment for microbial growth.
What is Biofilm and Why Does It Form?
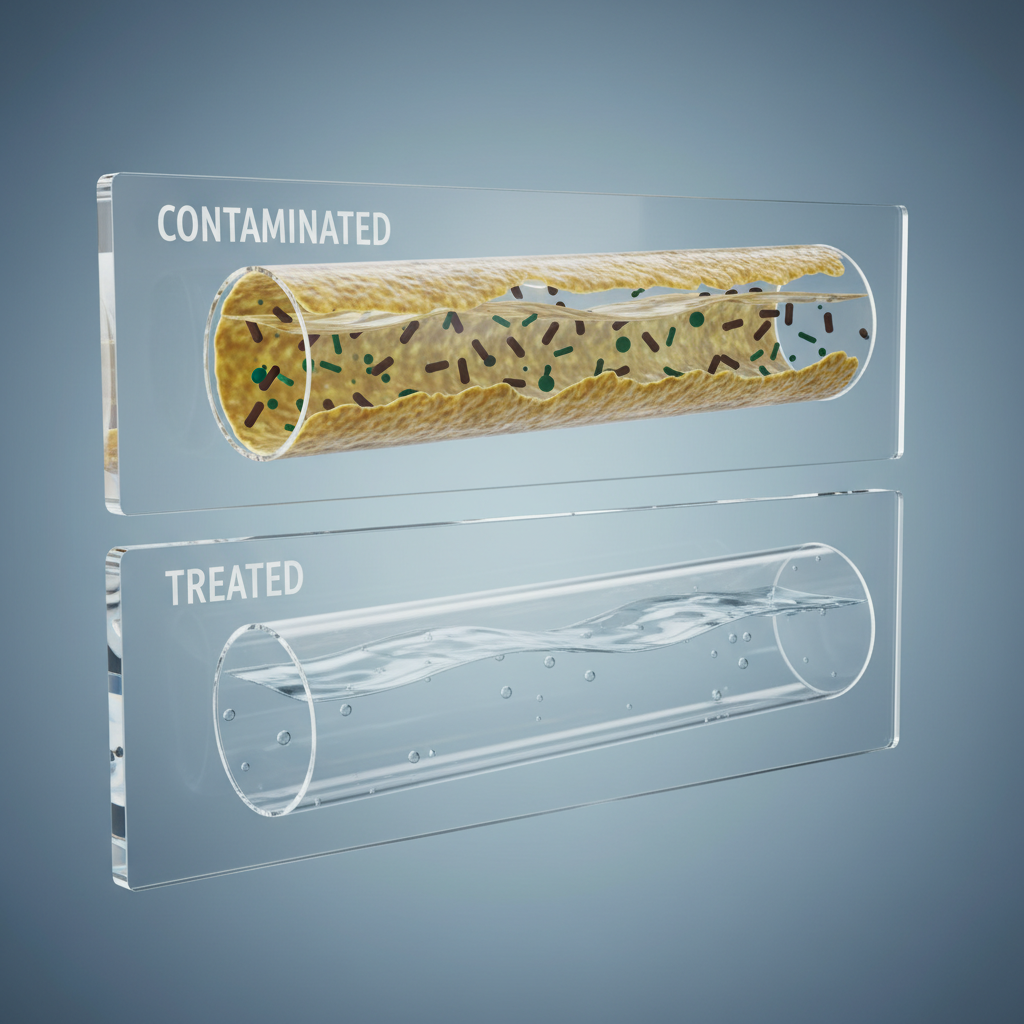
Biofilm is a complex community of microorganisms, primarily bacteria, that attach to surfaces and encase themselves in a slimy, protective matrix. This matrix makes them highly resistant to disinfection. In DUWLs, bacteria from incoming municipal water can attach to the tubing walls, multiply, and form a mature biofilm in a matter of weeks. Stagnation, particularly over weekends or holidays, accelerates this process dramatically, often leading to sharp spikes in microbial counts.
The risks associated with contaminated waterlines are well-documented. Pathogens such as Legionella pneumophila, Pseudomonas aeruginosa, and various non-tuberculous mycobacteria can thrive in these systems. Research available through resources like PubMed has consistently highlighted the potential for these organisms to cause infections, particularly in immunocompromised patients. This underscores the clinical urgency of maintaining water quality.
Regulatory and Quality Standards
Ensuring the safety of medical devices is a core regulatory principle. In the United States, the Food and Drug Administration (FDA) outlines stringent quality system regulations for medical device manufacturing. For clinics, this translates to an expectation that equipment is maintained to prevent patient harm. Similarly, international standards like ISO 13485:2016 for quality management systems emphasize risk management throughout a device’s lifecycle, including its use in a clinical setting. Adhering to a robust waterline management protocol is a key part of this quality assurance.
Core Strategies for Effective Waterline Management
A successful waterline maintenance program is not a single action but a consistent, multi-layered strategy. It combines daily physical processes with periodic chemical treatments to disrupt biofilm at every stage of its development.
Debunking a Common Misconception: The Flushing Fallacy
A prevalent myth in dental practices is that flushing waterlines between patients is enough to keep them clean. While flushing for 20-30 seconds is a critical step that helps reduce the planktonic (free-floating) microbial load, it does very little to remove established biofilm. The protective matrix of the biofilm is too adherent to be dislodged by water flow alone. Relying solely on flushing creates a false sense of security while the underlying contamination continues to grow.
A Structured Maintenance Protocol
To effectively manage DUWLs, clinics should implement a clear and consistent schedule. This structured approach ensures that no steps are missed and that the system is controlled proactively.
| Frequency | Action | Purpose | Key Considerations |
|---|---|---|---|
| Beginning of Day | Flush all lines for 2 minutes. | Clears stagnant water that has been sitting overnight. | |
| Between Patients | Flush all lines for 20-30 seconds. | Reduces planktonic microorganisms introduced during the previous procedure. | This is a critical step in reducing cross-contamination risk. |
| End of Day | Purge lines with air and/or follow manufacturer instructions for an overnight treatment. | Dries the lines to inhibit microbial growth overnight. | |
| Weekly | Administer a chemical “shock” treatment or use a continuous treatment product. | Kills bacteria and breaks down the biofilm matrix. | Always follow the specific instructions and contact time for the chemical agent used. |
| Quarterly/As Needed | Conduct water quality testing. | Verifies that the protocol is effective and that water meets safety standards (e.g., <500 CFU/mL). |
Expert Warning: The Danger of Stagnation
Practitioner-level experience consistently shows that periods of low use, such as long weekends or clinic holidays, are the most dangerous times for biofilm proliferation. In stagnant water, microbial counts can multiply exponentially. It is crucial to perform a thorough, extended flush upon returning to the clinic after any period of inactivity. Some protocols may even recommend a light chemical shock treatment after a vacation period to reset the lines.
Technologies for Advanced Waterline Disinfection
Modern dental chairs often incorporate features designed to simplify and automate waterline maintenance. Understanding these technologies can help a practice choose equipment that enhances both efficiency and safety. Many of these systems are central to the key tech in dental chairs for better patient care.
Independent Water Bottle Systems
This is the most fundamental feature for controlling water quality. An independent reservoir allows the clinic to bypass municipal water entirely, instead using distilled, sterile, or otherwise treated water. This provides a clean starting point and is a prerequisite for most chemical treatment and disinfection protocols. It also isolates the chair from any fluctuations or contamination events in the public water supply.
Automated Maintenance and Integrated Treatment
Higher-end dental units may feature automated systems that flush the lines at the push of a button or even run maintenance cycles automatically at the end of the day. Some systems are designed for continuous chemical treatment, where a low-level disinfecting agent is introduced into the water supply to consistently suppress microbial growth. These integrated solutions help ensure compliance by making the protocol easier to follow.
Filtration and Purification
Several technologies aim to treat water just before it reaches the patient:
- Microfiltration: Inline 0.2–0.45 µm filters can be installed to capture bacteria and particulates before they enter the handpiece or air/water syringe. While effective, these filters do not treat the water within the lines themselves, and they require regular replacement (typically every 6-12 months) as they can become clogged.
- Chemical Neutralization: Some systems use agents that neutralize harmful chemicals, which can be beneficial when using certain potent disinfectants.
- Ultraviolet (UV) Sterilization: Though less common in chairside applications, UV light can be an effective method for killing microorganisms in water as it passes through a sterilization chamber.
Monitoring and Verification: Ensuring Your Protocols Work
Implementing a protocol is only half the battle; the other half is verifying that it works. Regular testing provides the data needed to confirm your water is safe and to identify any potential issues before they become serious problems.
Pro Tip: Tailor Monitoring Cadence to Risk
Not all clinics face the same level of risk. A standard clinic can typically test its waterlines quarterly. However, high-volume practices or those that regularly treat immunocompromised patients should consider a more frequent, monthly testing schedule. This risk-based approach ensures the highest level of safety for the most vulnerable populations.
Water Quality Testing Methods
There are two primary methods for testing your DUWLs:
- In-Office Test Kits: These kits are convenient and provide a quick estimate of the microbial load. They typically involve collecting a water sample, plating it on a culture medium, and incubating it for a set period. While useful for regular screening, they may not be as precise as laboratory testing.
- Third-Party Laboratory Testing: This is the gold standard for accuracy. A water sample is collected according to the lab’s instructions and mailed for analysis. The lab provides a detailed report with a precise colony-forming unit (CFU/mL) count. This method is essential for initial validation of a new protocol and for investigating a failed in-office test.
The Importance of Documentation and Training
All waterline maintenance activities and test results must be meticulously documented. This logbook is critical for demonstrating compliance during inspections and for tracking trends over time. Creating a clear Standard Operating Procedure (SOP) and ensuring all staff are trained on proper techniques—from chemical handling to water sampling—is fundamental. Incorrect sampling, for instance, can easily lead to a false negative, masking a real contamination problem. A well-documented and well-executed plan is a cornerstone of a clinic’s commitment to infection control and overall financial health, as explained in how chair durability impacts your clinic’s financial health.
Wrapping Up: Building a Culture of Waterline Safety
Managing dental unit waterlines is a non-negotiable aspect of modern dental practice. It is a critical component of infection control that directly impacts patient safety and a clinic’s reputation. The threat of biofilm is persistent, but it is manageable with a systematic, multi-pronged approach.
The key takeaways are clear: daily flushing is necessary but insufficient on its own. It must be combined with regular chemical treatments to remove biofilm, periodic shock treatments to reset the system, and consistent monitoring to verify effectiveness. By embracing this comprehensive strategy and investing in equipment with modern maintenance features, clinics can ensure their waterlines are a conduit for care, not a source of contamination.
Disclaimer: This article is for informational purposes only and does not constitute professional medical or regulatory advice. Dental practices should always consult their equipment manufacturer’s instructions for use and adhere to the guidelines set forth by local and national regulatory bodies.
References:






