How Chair Design Impacts Infection Control & Hygiene
The Unseen Impact of Dental Chair Design on Patient Safety
Seamless upholstery and minimalist designs are not just about aesthetics; they are crucial for effective infection control. While sterilization protocols and disposable instruments are front and center in dental hygiene, the very chair the patient sits in can be a hidden reservoir for contaminants. The design of a dental chair directly impacts how easily and effectively it can be cleaned, making specific design choices fundamental to enhancing patient safety and operational efficiency.
Every seam, crevice, and material choice can either support or undermine a clinic’s hygiene protocols. For busy dental practices, where time between appointments is limited, a chair that is difficult to clean presents a significant risk. This article explores how specific design elements of dental chairs play a critical role in infection control and offers a practical framework for evaluating them.
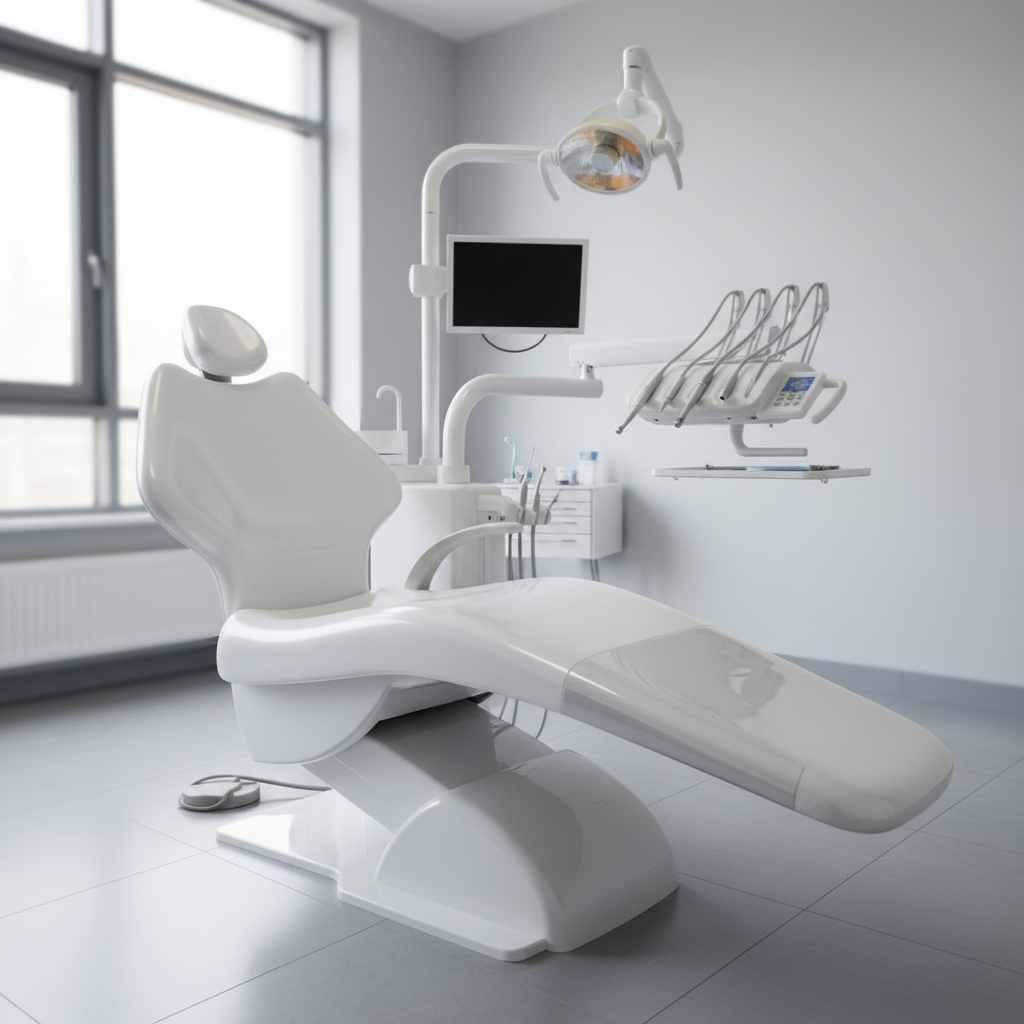
Anatomy of a Hygienic Dental Chair
A chair’s defense against contamination begins with its physical construction. Surfaces that are easy to clean and materials that withstand rigorous disinfection are the cornerstones of a hygienic design. This goes beyond the surface level, involving the very way the chair is assembled and shaped.
Upholstery and Seams: The First Line of Defense
Traditional dental chairs often feature stitched or tufted upholstery. While this may provide a certain look, these seams are a major liability for infection control. Experienced clinic technicians report that narrow seams and hidden fasteners are notorious for trapping fluids, debris, and biofilm. Once contaminants are in these crevices, they are incredibly difficult to remove, creating a persistent source of potential cross-contamination.
A far superior approach is the use of seamless or minimally seamed upholstery. Modern manufacturing techniques allow for continuous surfaces with heat-sealed or welded seams. This eliminates the hiding spots for bacteria and viruses, allowing for a smooth, unbroken surface that can be wiped clean in seconds. Our analysis indicates that chairs with seamless upholstery can reduce cleaning time between patients by an estimated 20-30%, a significant efficiency gain in a busy clinic.
Material Durability and Disinfectant Compatibility
The material of the upholstery is just as important as its seam design. It must be non-porous to prevent the absorption of fluids and resistant to staining. Crucially, it must also be certified for compatibility with common hospital-grade disinfectants, such as those containing alcohols or quaternary ammonium compounds (quats).
A common mistake is using abrasive cleaners or incompatible chemical agents. This can cause micro-abrasions on the surface of the upholstery. While invisible to the naked eye, these tiny scratches create new havens for microbes and can accelerate the breakdown of the material, leading to cracks and tears where contaminants can penetrate deeper. For instance, repeated use of high-chlorine solutions on chrome-plated parts can cause corrosion, creating rough surfaces that are difficult to sterilize.
Shape and Accessibility: Designing for Cleanability
The overall shape of the chair influences how easily it can be cleaned. Designs with complex angles, tight junctions, and hidden areas are inherently difficult to wipe down effectively. In contrast, chairs designed with smooth contours and open spaces allow for complete access.
A practical design heuristic is to prefer corners with a radius of at least 3–5 millimeters. This small detail ensures that a disinfectant wipe can maintain full contact with the surface, preventing the “bridging” effect that occurs when a wipe misses the sharp inner corner of a 90-degree angle. Likewise, ensuring there is adequate space around motors, lifts, and control panels allows staff to clean these critical areas thoroughly.
Key Design Features That Simplify Cleaning Workflows
Beyond the primary surfaces, specific features can either streamline or complicate daily hygiene protocols. Thoughtful design anticipates the needs of the clinical team and builds solutions directly into the chair itself.
The Myth of “Any Disinfectant Will Do”
A common misconception in clinic hygiene is that a stronger disinfectant is always better. In reality, material compatibility is key. Using a disinfectant that is not approved by the chair manufacturer can lead to material degradation, voiding the warranty and, more importantly, compromising the hygienic integrity of the chair. For example, some high-concentration alcohol solutions can dry out and crack certain types of upholstery over time. Always follow the manufacturer’s guidelines for approved cleaning agents and, critically, adhere to the specified dwell times. Over-application or insufficient contact time can be just as problematic as using the wrong chemical.
Removable and Autoclavable Components
Certain parts of a dental chair, like headrests and armrests, are high-touch areas. Designs that feature removable headrest cushions and armrest covers offer a significant advantage. These components can be quickly swapped out between patients and, if made from appropriate materials, can be sterilized in an autoclave for maximum assurance. This modularity not only enhances infection control but also simplifies maintenance and replacement, extending the life of the chair.
Integrated Systems and Serviceability
Well-designed chairs often feature integrated utility boxes and internal routing for water and air lines. This minimizes the number of external hoses and connections that can collect dust and contaminants. Furthermore, easy access to service panels and replaceable seals is a critical feature. It allows technicians to perform maintenance without compromising the chair’s internal electronics and mechanisms. A properly sealed base and motor shroud prevent fluid ingress from spills or cleaning, a common cause of equipment failure and a hidden hygiene risk.
A Practical Framework for Dental Chair Hygiene
To ensure consistent and effective infection control, clinics should implement a structured cleaning protocol based on the chair’s design. This transforms routine cleaning from a repetitive task into a systematic process.

Here is a sample workflow that can be adapted for any clinical setting:
Dental Chair Hygiene Protocol
| Frequency | Task | Key Areas & Rationale |
|---|---|---|
| Between Patients | Top-to-Bottom Wipe-Down | 1. Headrest: Highest contact point. 2. Armrests: Frequent patient and operator contact. 3. Upholstery: Full surface wipe, paying attention to leg and back areas. 4. Controls: Disinfect all buttons, switches, and touchpads. 5. Base: Wipe down the chair base and surrounding floor area. This top-to-bottom sequence prevents dripping from a dirty area onto a just-cleaned one. |
| Weekly | Targeted Deep Clean | 1. Drains & Filters: Clean and disinfect suction system lines and traps to prevent biofilm buildup. 2. Joints & Seams: Use a soft brush to gently clean any unavoidable seams or joints. 3. Casters/Wheels: Remove any trapped hair or debris. |
| Monthly | Upholstery & Systems Inspection | 1. Inspect for Damage: Carefully check all upholstery for any signs of cracking, peeling, or abrasion. Document and schedule repairs immediately. 2. Check Seals: Ensure all gaskets and seals around the base and utility connections are intact to prevent fluid ingress. |
Adhering to Global Standards for Trust and Safety
Manufacturing dental equipment for a global market requires adherence to stringent regulatory standards. These regulations are not just bureaucratic hurdles; they are essential frameworks for ensuring product safety and quality. For example, compliance with ISO 13485:2016 demonstrates a manufacturer’s commitment to a quality management system specifically for medical devices.
For products sold in the European Union, a CE Marking is mandatory, signifying that the product meets high safety, health, and environmental protection requirements. Similarly, entry into the U.S. market requires adherence to the FDA’s Quality System Regulation under 21 CFR Part 820, which governs the design, manufacturing, and distribution of medical devices.
These standards implicitly cover hygienic design. A chair that is difficult to clean or breaks down under normal disinfection protocols would likely fail the risk analysis required by these regulatory bodies. Therefore, choosing a chair from a manufacturer with a proven record of compliance provides an additional layer of trust and assurance.
Key Takeaways
The design of a dental chair is a fundamental component of a clinic’s infection control strategy. To enhance patient safety and improve efficiency, dental professionals should prioritize chairs that are engineered for hygiene.
- Favor Seamless Design: Opt for chairs with smooth, seamless upholstery to eliminate hiding places for bacteria and biofilm.
- Verify Material Resilience: Ensure the chair’s materials are non-porous and certified to withstand hospital-grade disinfectants without degrading.
- Look for Cleanable Shapes: Choose designs with rounded corners and good access to all areas, making thorough cleaning faster and more effective.
- Prioritize Smart Features: Removable components and easily serviceable parts not only improve hygiene but also contribute to the long-term value and reliability of the equipment.
By viewing dental chair selection through the lens of infection control, clinics can make a smarter investment in patient safety, staff efficiency, and long-term operational success.
Disclaimer: This article is for informational purposes only and does not constitute professional medical advice or a substitute for professional consultation. Dental professionals should always adhere to the specific cleaning and maintenance protocols provided by the equipment manufacturer and comply with all local and national infection control regulations.





