Touchless Controls in Modern Dental Lighting
The Unseen Advantage: How Touchless Controls Are Redefining Dental Lighting
In modern dental practice, the margin for error is vanishingly small. This precision extends beyond clinical procedures to the very environment where care is delivered. Infection control is a cornerstone of patient safety, and every surface, tool, and workflow is scrutinized to minimize cross-contamination. For years, the operatory light, a critical component for diagnostic accuracy, remained a frequent point of manual contact. Adjusting intensity or position required a clinician to stop, touch the fixture, and potentially compromise sterile protocols.
Hands-free operation, powered by motion-activated sensors and other touchless technologies, is transforming this dynamic. These systems are no longer a novelty but a fundamental component of a modern, hygienic, and efficient dental practice. By eliminating the need for manual adjustments, touchless lighting directly supports robust infection control protocols, allowing clinicians to maintain focus and sterility throughout a procedure. This article explores the technology behind touchless dental lights, the significant clinical benefits they offer, and the practical steps for successful implementation.
The Technology Driving Hands-Free Illumination
The magic of touchless control lies in sophisticated sensors that translate movement or presence into commands. While the user experience is seamless, the underlying technology is a product of careful engineering designed for the specific demands of a clinical environment.
Understanding Sensor Technology: PIR vs. Proximity
Most motion-activated dental lights rely on Passive Infrared (PIR) sensors. These sensors detect the infrared energy (heat) emitted by a person’s body. When a hand or body moves into the sensor’s detection zone, it triggers a change in the infrared landscape, which the sensor interprets as a command to turn the light on, off, or adjust its settings. PIR sensors are well-suited for this role because they are not easily fooled by inanimate objects moving, reducing the chance of false activations.
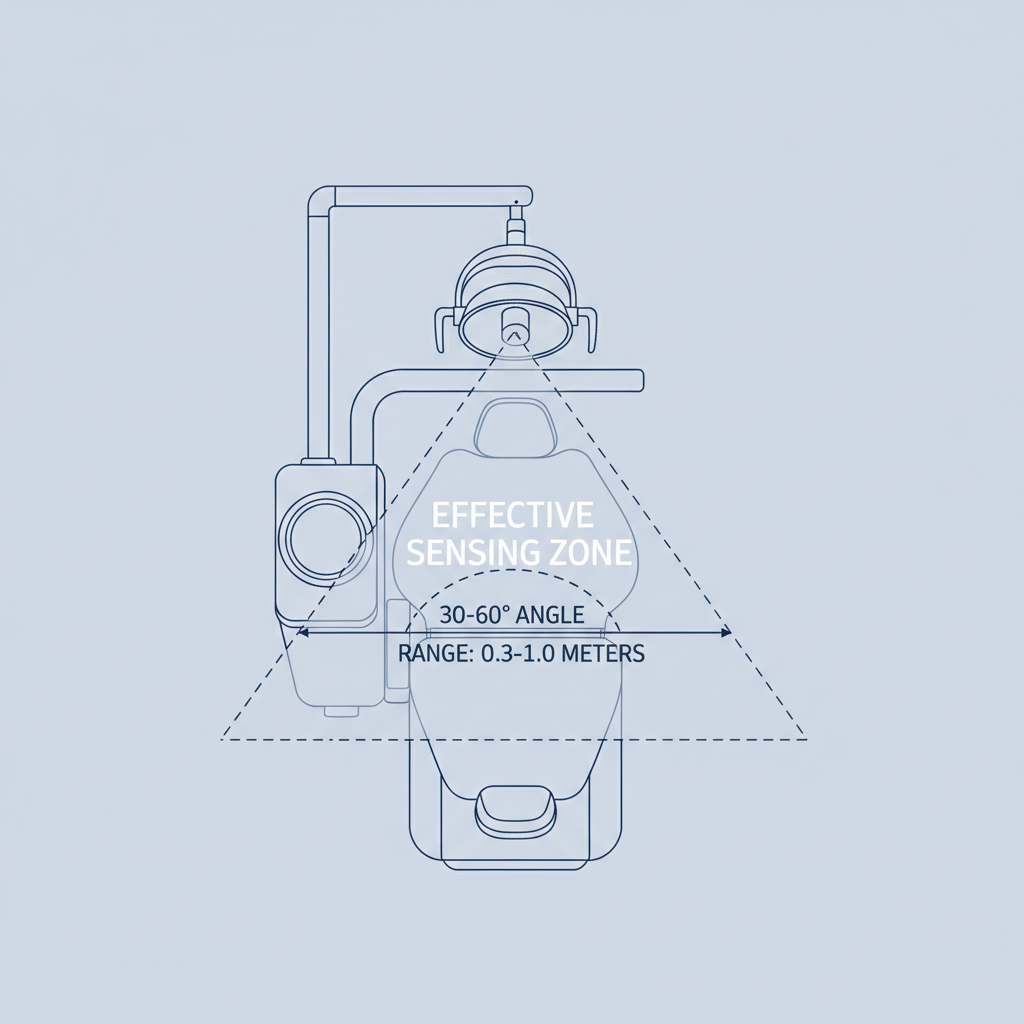
A common mistake I’ve seen in clinics is improper sensor setup, leading to frustration. A sensor mounted at an awkward angle can be triggered by the clinician’s head movement, while an overly sensitive setting might activate the light whenever someone walks across the room. The key is precise calibration. For optimal performance, the detection range should be set to approximately 0.3 to 1.0 meters, with the detection cone restricted to a 30 to 60-degree field. This creates a responsive zone directly in front of the clinician without picking up extraneous movement.
System Responsiveness and the Feel of Control
For touchless technology to be effective, it must feel instantaneous. Any perceptible delay, or latency, between a gesture and the light’s response can disrupt a clinician’s workflow. The goal is to achieve a system latency under 250–350 milliseconds. This threshold ensures the light reacts as quickly as a manual switch, making the interaction feel natural and immediate. This level of responsiveness is crucial for maintaining focus during complex procedures where seamless environmental control is paramount.
Clinical Benefits Beyond a Sterile Field
While enhanced infection control is the primary driver for adopting touchless lighting, the benefits extend deep into clinical workflow, diagnostic accuracy, and operational efficiency. The technology acts as a silent partner, streamlining tasks and improving the quality of care.
Myth Debunked: Touchless Tech is Not an Automatic Fix
A common misconception is that installing a motion-activated light is a complete solution for infection control. My experience, and that of many clinicians I’ve worked with, shows this isn’t the case. Touchless lights are a powerful tool, but they deliver maximum benefit only when integrated into a broader strategy. The true gains in safety and efficiency come from combining the technology with updated staff protocols and training. For a deeper dive into this synergy, see our guide on Tech Integration and Infection Control in Chairs. The hardware reduces contact points, but the team’s workflow is what solidifies the sterile chain.
Superior Illumination for Uncompromising Diagnostic Accuracy
The quality of light is as important as its control. Modern LED fixtures offer remarkable control over two critical metrics: color temperature and Color Rendering Index (CRI).
- Color Temperature: Measured in Kelvin (K), this determines if the light appears warm (yellowish) or cool (bluish). For dental work, a tunable range of 3500–5000 K is ideal. This spectrum allows clinicians to simulate different lighting conditions, from natural daylight to indoor light, ensuring that restorations and shade matching are accurate in any environment.
- Color Rendering Index (CRI): This scale, from 0 to 100, measures how accurately a light source reveals the true colors of an object. For clinical applications, a CRI of 90 or above is the standard. This high fidelity ensures that the subtle shades of tissue and enamel are clearly distinguishable, which is critical for accurate diagnostics and aesthetic dentistry.
Another technical aspect that impacts quality is flicker. Some lower-quality LED dimming systems use a method called Pulse Width Modulation (PWM) at a low frequency, which can create a subliminal flicker. This can cause eye strain and fatigue over long procedures. To avoid this, it’s best to choose systems that use high-frequency PWM (above 2 kHz) or constant-current drivers, which provide smooth, flicker-free dimming across all intensity levels.

A Practical Guide to Implementation and Maintenance
Selecting the right technology is only the first step. Proper installation, calibration, and long-term maintenance are essential to unlocking the full potential of a touchless lighting system and ensuring it remains a reliable asset.
Installation and Calibration Checklist
To avoid common pitfalls, I recommend a structured approach to setup. A small investment of time in calibration prevents countless frustrations down the line. It’s a process of tuning the equipment to the unique dimensions and workflow of your specific operatory.
| Step | Best Practice | Rationale |
|---|---|---|
| 1. Sensor Placement | Mount the sensor so its detection zone covers the intended user’s hand-gesture area without intersecting with the clinician’s head or torso during normal operation. | Prevents false activations from routine movements, ensuring the light responds only when intended. |
| 2. Range & Cone Tuning | Calibrate the detection range to 0.3–1.0 m and the cone angle to 30–60°. | Creates a focused and responsive activation zone, minimizing triggers from background activity. |
| 3. Sensitivity Adjustment | Start with the lowest sensitivity setting and gradually increase it until it reliably detects deliberate gestures without triggering from minor movements. | Balances responsiveness with stability, ensuring the system is helpful, not disruptive. |
| 4. Manual Override Test | Always confirm that the manual override and any footswitch fallbacks are functioning correctly. | Guarantees that the light remains fully operational in any scenario, providing crucial system redundancy. |
| 5. EMI Check | Ensure wireless control modules are not placed near high-power wiring, such as for dental micromotors. | Reduces the risk of electromagnetic interference (EMI), which can disrupt sensor performance and reliability. |
Long-Term Reliability and Maintenance
Durability is a key purchasing consideration for any dental equipment. For touchless lighting, this means focusing on the components most exposed to the clinical environment. The sensor modules should be sealed to protect against dust and moisture, ideally with an IP (Ingress Protection) rating of IP54 to IP65.
Furthermore, control modules should be easily accessible for any potential firmware updates or sensor replacements. Like any precision instrument, periodic recalibration is good practice. In high-use clinics, a quick validation of sensor accuracy every 6 to 12 months can ensure the system continues to perform as expected. This proactive approach to maintenance is a small investment that pays dividends in reliability and longevity.
Ensuring Compliance and Future-Proofing Your Investment
Investing in new operatory technology requires careful consideration of regulatory compliance and long-term value. Touchless lighting systems, as medical devices, must adhere to stringent quality and safety standards.
Navigating Key Regulatory Standards
When sourcing equipment, verifying its compliance is non-negotiable. Reputable manufacturers design and build their products within a robust quality management framework. The foundational standard for this is ISO 13485:2016 – Quality Management Systems, which ensures that a manufacturer has proven processes for designing, producing, and distributing medical devices safely.
Beyond this, products must meet the specific requirements of the markets where they are sold. For equipment intended for the European Union, this means it must carry the CE Marking – European Conformity, signifying compliance with EU safety, health, and environmental protection requirements. In the United States, the Food and Drug Administration (FDA) sets the rules. Devices must comply with regulations such as the FDA 21 CFR Part 820, which governs quality system regulation. Partnering with suppliers who can provide clear documentation of these certifications is essential for ensuring you are investing in equipment that is both safe and legal to operate.
Smart Design for a Connected Future
Touchless control is a key feature in the broader trend toward integrated, digital dentistry. As operatories become more connected, the ability of different systems to work together becomes increasingly important. When considering a new lighting system, think about its place within your practice’s technology ecosystem. Features like a manual override or footswitch compatibility provide essential backup, ensuring uninterrupted operation. This focus on how digital dentistry transforms the dental chair is central to building a practice that is both efficient and resilient.
Wrapping Up: A Clearer, Safer Path Forward
Touchless controls in dental lighting represent a significant step forward in operatory design. By removing a key point of manual contact, they directly enhance infection control protocols and promote a safer environment for both patients and clinicians. But the advantages don’t stop there. These systems improve clinical workflow, reduce procedure times, and provide superior illumination that leads to better diagnostic and aesthetic outcomes.
However, technology alone is not a panacea. Realizing these benefits requires a holistic approach. It demands careful selection of high-quality, compliant equipment, precise installation and calibration, and the integration of the technology into team-wide hygiene protocols. By focusing on these key areas, dental practices can leverage touchless lighting to create a smarter, safer, and more efficient clinical environment.
Disclaimer: This article is for informational purposes only and does not constitute professional medical or regulatory advice. Dental professionals should consult with qualified experts and regulatory bodies to ensure compliance and patient safety.






